Brings relief to a wide range of dry skin conditions
Experience the E45 Effect
Reviews




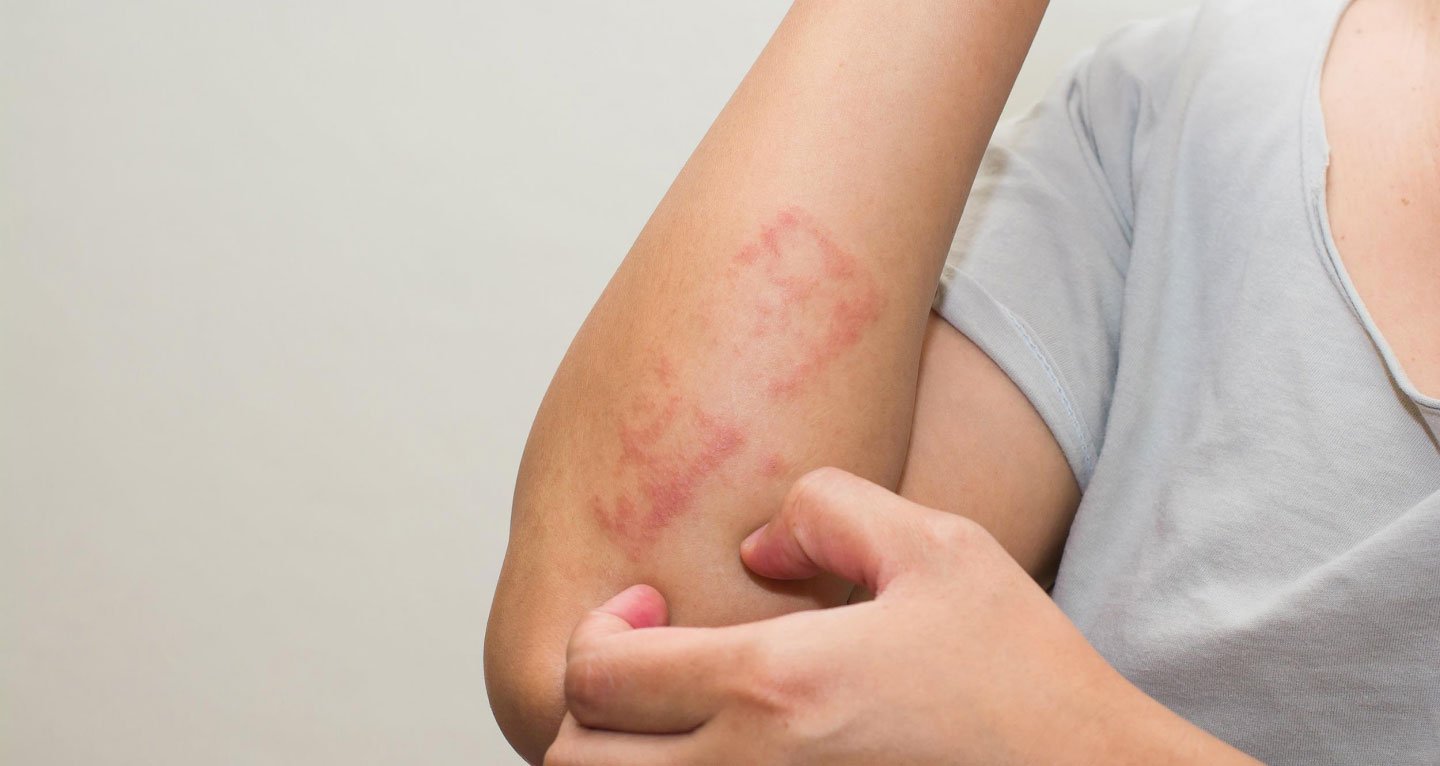
Eczema
Eczema is a skin condition where patches of skin can become dry, itchy, inflamed, cracked and sore: often affects hands, elbows, knees, face and/or scalp. It can be treated.
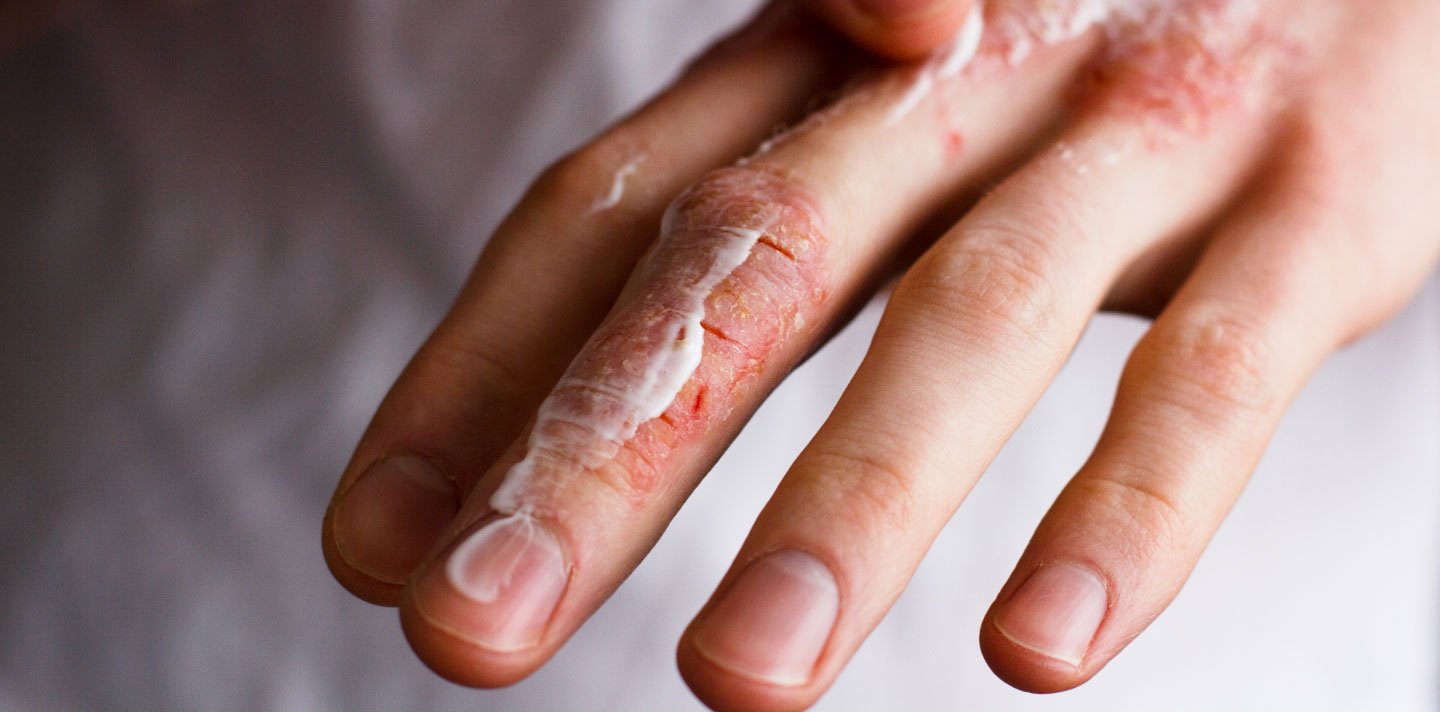
Itchy Skin
Itchy skin is common and can affect any part of the body. It causes the skin to be less effective as a natural barrier. It can be helped.

How to use an emollient?
Emollients should be applied regularly. They help the skin retain moisture by creating a protective film and in maintaining the skin’s pH.
*Source: Nielsen, Total Coverage, Skin Treatment, w/e 13.08.22




























